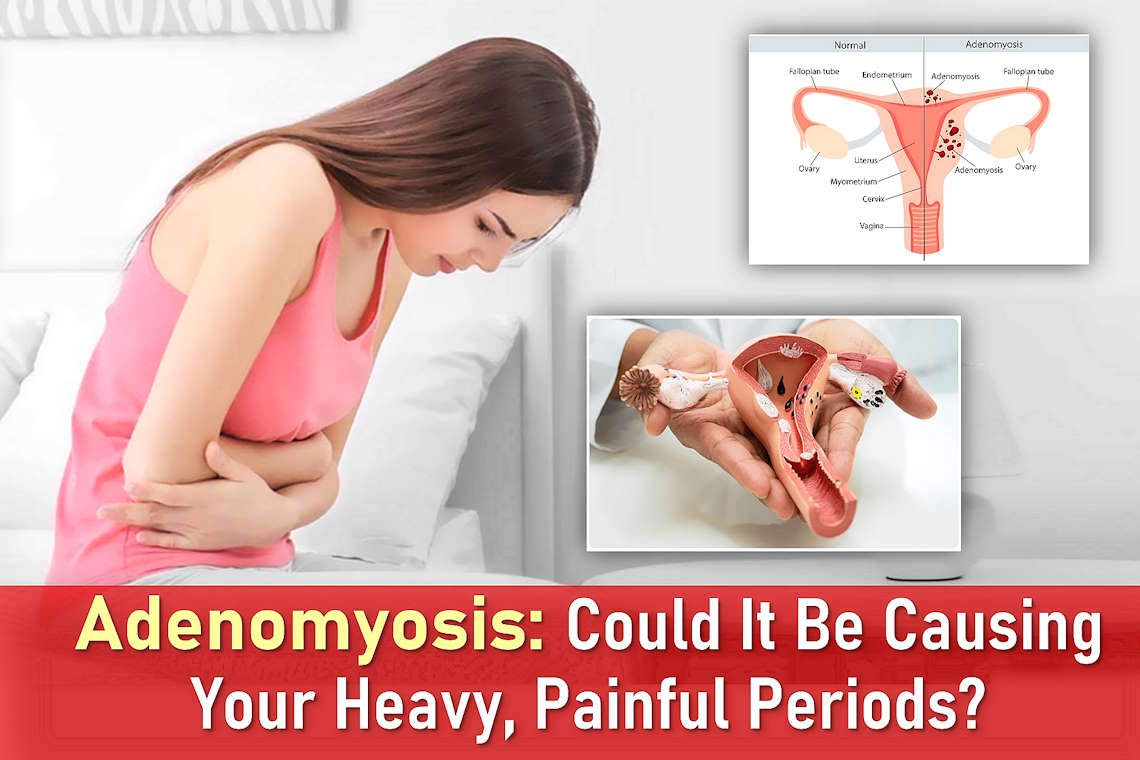
Adenomyosis: Could It Be Causing Your Heavy, Painful Periods?
For many women, menstrual cramps and heavy bleeding are an expected, though unpleasant, part of life. These symptoms are often managed with pain relievers, heating pads, or rest. However, when periods become unusually heavy or painful to the point that they interfere with daily activities, it may signal an underlying condition. One possible explanation is a condition called adenomyosis.
What is Adenomyosis?
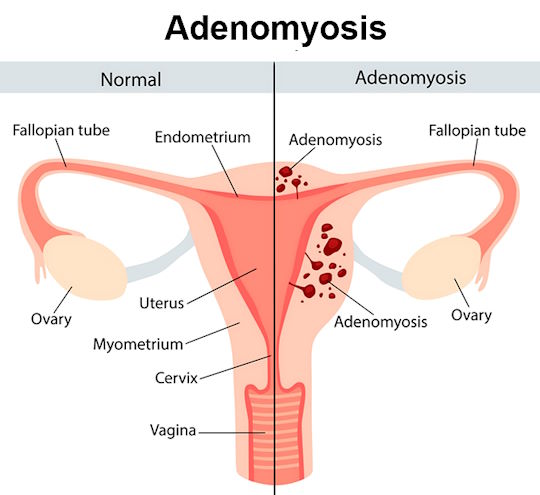
To understand what is adenomyosis, it helps to look at the basic structure of the uterus. The uterus has an inner lining called the endometrium, which builds up each month and sheds during menstruation. The outer layer is made of thick muscle. In a healthy uterus, these layers remain separate.
With uterine adenomyosis, this separation breaks down. Cells from the endometrium grow into the muscular wall of the uterus, where they do not belong. Each month, these misplaced cells respond to hormonal changes just like the normal lining, thickening and bleeding. But because they are trapped inside the muscle, the blood cannot exit the body. This leads to inflammation, swelling, and pain. Over time, the adenomyosis uterus often becomes enlarged and tender.
How Common is This Condition?
Adenomyosis is more common than many people realize. Studies suggest it may affect anywhere from 20% to over 80% of women with symptoms, with an average of about one in three. It is most often diagnosed in women in their 30s and 40s, though it can also affect women in their 50s.
These figures may actually underestimate its prevalence. In the past, adenomyosis was often confirmed only after a hysterectomy, when tissue could be studied under a microscope. Many women with symptoms likely went undiagnosed. Today, improved imaging, such as an ultrasound, makes it possible to identify the condition without surgery, helping more women receive timely answers.
Adenomyosis vs Endometriosis
Because both conditions involve tissue similar to the endometrium growing where it should not, people often compare adenomyosis vs endometriosis. The main difference is location. In endometriosis, tissue grows outside the uterus, often affecting the ovaries, fallopian tubes, bladder, or intestines. In adenomyosis, the tissue grows inward, burrowing into the muscle wall of the uterus (the myometrium).
Endometriosis is more commonly diagnosed in younger women, while adenomyosis is usually found in women later in their reproductive years. It is also possible for someone to have both conditions at the same time.
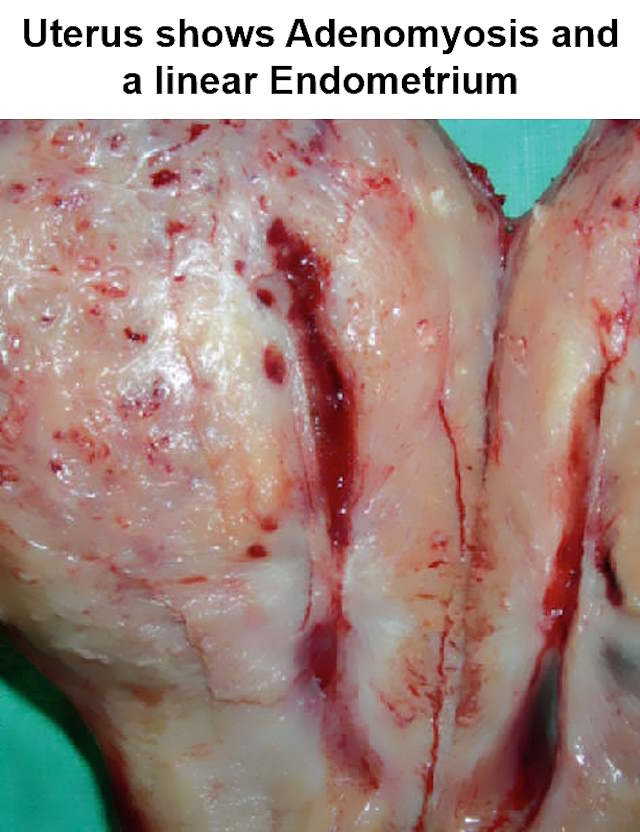
Common Adenomyosis Symptoms
The adenomyosis symptoms vary widely. Some women have no symptoms and only learn about the condition during exams for other reasons. Others experience symptoms so severe that daily life becomes difficult.
Common symptoms include:
- Very heavy or prolonged menstrual bleeding (menorrhagia).
- Severe cramps during periods (dysmenorrhea), often worsening over time.
- Chronic pelvic pain that may persist throughout the month.
- Pain during sexual intercourse (dyspareunia).
- Bloating or pressure in the lower abdomen, sometimes described as “adenomyosis belly.”
- An enlarged uterus, which may feel like a firm mass in the lower abdomen.
- Pressure on nearby organs, leading to frequent urination or constipation.
There is some relief in knowing that because adenomyosis is driven by estrogen, its symptoms usually lessen or disappear after menopause, when estrogen levels naturally decline.
Why Adenomyosis Often Goes Unrecognized
If you have never heard of adenomyosis, you are not alone. For years, this condition has remained largely overlooked. One reason is the widespread belief that painful or heavy periods are simply a normal part of life. Many women are told from a young age that severe cramps or heavy bleeding are “just part of being a woman” or something that runs in the family. This mindset can prevent women from seeking help, leaving them to cope with symptoms in silence.
Even when medical care is sought, the condition can still go undetected. Doctors often start with standard treatments such as birth control pills to control bleeding and pain, without necessarily ordering specialized imaging. Since more common conditions like fibroids are usually suspected first, adenomyosis may be overlooked. To complicate matters further, its symptoms are similar to many other pelvic disorders, making it difficult to diagnose without targeted evaluation.
The encouraging news is that awareness is improving. More healthcare providers now recognize the signs of adenomyosis, and advances in imaging technology are making diagnosis easier. An ultrasound is a valuable tool for detection. Getting an accurate diagnosis is the essential first step toward accessing proper adenomyosis treatment and regaining quality of life.
Potential Causes of Adenomyosis
Researchers have not identified a single cause of uterine adenomyosis, but several theories help explain its development.
One leading explanation is the tissue injury and repair theory. Events that disturb the boundary between the endometrium and uterine muscle, such as a cesarean section, dilation and curettage (D&C), or pregnancy, may allow endometrial cells to enter the muscle wall, where they take root and grow.
Another theory points to development before birth. Some experts believe certain women may be predisposed because endometrial tissue is misplaced during fetal development. Hormones also play an important role, as estrogen, progesterone, and prolactin can stimulate the growth of this tissue. Research is also exploring whether the immune system may contribute by failing to stop these cells from implanting in the muscle wall.
It is important to emphasize that adenomyosis is not caused by anything you did or did not do. Lifestyle choices do not lead to the condition, and at present, there is no known way to prevent it.
How Adenomyosis is Diagnosed
For many women, reaching an adenomyosis diagnosis can be a long and frustrating journey. The symptoms are varied and can mimic other issues such as pelvic inflammatory disease or irritable bowel syndrome. Some women endure the pain for years, assuming it is normal, before receiving answers.
This delay can have real consequences. Chronic heavy bleeding can cause iron-deficiency anemia, leading to exhaustion, weakness, and shortness of breath. Living with constant pain and unpredictable bleeding can also affect mental health, relationships, work, and social life.
Diagnosis usually begins with a detailed discussion of symptoms and a pelvic exam. A doctor may notice that the uterus feels enlarged, soft, or tender. The most effective tool for diagnosis is imaging, with transvaginal ultrasound often used first. A trained specialist looks for changes in the uterine wall, such as small cysts, uneven thickness, or a speckled appearance. In more complex cases, magnetic resonance imaging (MRI) can provide a clearer picture and help rule out other conditions, giving a more definitive diagnosis.
Adenomyosis Treatment and Management
Managing adenomyosis is a personal journey, shaped by the severity of your symptoms, your age, and your plans for future pregnancy. The main goal of adenomyosis treatment is to reduce heavy bleeding and pain so you can live more comfortably. For women nearing menopause, when symptoms often ease naturally, careful monitoring may be an option if symptoms are mild. However, if your daily life is being disrupted, exploring treatment is important.
Medical Management with Adenomyosis Medication
Most women begin with adenomyosis medication to help manage symptoms. These treatments focus on easing pain and regulating hormones that drive the condition.
- Anti-inflammatory drugs (NSAIDs): Over-the-counter options like ibuprofen or naproxen can reduce inflammation and menstrual cramps. They work best when started a day or two before bleeding begins.
- Hormonal therapies: Because adenomyosis is influenced by estrogen, treatments that lower estrogen levels or stop ovulation can ease symptoms. Options include progestin (dienogest), hormonal intrauterine devices (IUDs) that release progestin, continuous-use birth control pills, patches, or vaginal rings that suppress periods, and gonadotropin-releasing hormone (GnRH) agonists, which temporarily lower estrogen to shrink affected tissue.
Procedural and Surgical Adenomyosis Treatments
If medications are not enough, certain procedures or surgeries may be considered. Consulting a specialist, such as a gynecologist experienced in complex uterine conditions, is essential for finding the treatment that best matches your needs and future plans.
- Endometrial ablation: A procedure that removes or destroys the uterine lining to reduce heavy menstrual bleeding. It is not suitable for women who wish to have children and may be less effective if adenomyosis extends deeply into the uterine muscle.
- Uterine artery embolization (UAE): A minimally invasive treatment that blocks blood flow to the uterus, causing adenomyosis tissue to shrink. It may help preserve fertility, but its long-term impact on future pregnancies is still being studied.
- Adenomyomectomy: A surgical procedure useful for focal adenomyosis, where the diseased portion of the uterus is removed. It can improve pelvic pain and abnormal uterine bleeding (AUB), while preserving the uterus for women who still wish to conceive.
- Cytoreductive surgery: Involves extensive removal of adenomyosis tissue along with a portion of healthy uterine muscle (techniques include wedge resection, triple-flap method, or asymmetric dissection). This approach may significantly improve pelvic pain and AUB, but there can be some risks of obstetric complications in future pregnancies.
- Hysterectomy: The surgical removal of the uterus, considered the only permanent cure for adenomyosis. It is typically recommended when other treatments fail or when a woman has completed her family. This procedure completely resolves symptoms.
Adenomyosis, Fertility, and Pregnancy Outcomes
The relationship between adenomyosis and pregnancy is still being studied. While many women with adenomyosis conceive and carry healthy pregnancies, the condition can sometimes make conception more difficult. Changes in the uterine muscle and increased inflammation may interfere with embryo implantation or raise the risk of early miscarriage. Some studies also suggest a link with pregnancy complications such as preterm birth.
It is important to keep in mind that these risks are not guarantees. Many women with adenomyosis go on to have successful full-term pregnancies. If you have difficulty conceiving or have experienced pregnancy loss, consulting a fertility specialist (reproductive endocrinologist) can be helpful. They may use advanced imaging, such as an ultrasound, to assess your uterus and recommend strategies to improve your chances, including fertility treatments like IVF if needed.
Living with Adenomyosis: Prognosis
It is important to know that adenomyosis is a benign condition. It is not cancer and does not increase your risk of developing cancer. The main concern is the effect it can have on your daily life before menopause.
The overall outlook is positive, as there are many effective treatment options. Finding the right approach may take time, but relief is possible. After menopause, when estrogen levels drop, the condition usually resolves on its own. Until then, treatment focuses on managing symptoms so you can live more comfortably and without constant disruption from your periods.
Final Thoughts
If heavy, painful periods or persistent bloating that resembles an adenomyosis belly sound familiar, do not dismiss these symptoms as normal. You are your own best advocate. Keep track of your symptoms, schedule a visit with your gynecologist, and ask whether adenomyosis could be the cause. Inquire about the benefits of a pelvic ultrasound for diagnosis. With growing awareness and modern treatment options, you do not need to accept difficult periods as your fate. Effective help is available, and the first step is speaking up.
Frequently Asked Questions About Adenomyosis
Is adenomyosis a form of cancer?
No, adenomyosis is a benign (non-cancerous) condition. The tissue that grows into the uterine muscle is normal endometrial tissue, not cancer. It does not increase your risk of uterine cancer. Still, any unusual bleeding or pelvic pain should always be evaluated by a doctor to rule out other conditions.
What is the main difference between adenomyosis vs endometriosis?
The difference lies in the location of the tissue. In endometriosis vs adenomyosis, endometriosis means tissue grows outside the uterus, often on the ovaries, fallopian tubes, bladder, or intestines. In adenomyosis, the tissue grows within the muscular wall of the uterus itself. Some women may have both conditions at the same time.
Can you get pregnant with adenomyosis?
Yes, many women with adenomyosis conceive and have healthy pregnancies. However, the condition can sometimes make conception more difficult and may increase the risk of miscarriage or complications like preterm birth. If you are struggling to get pregnant, consulting a fertility specialist is recommended to create a plan tailored to your situation.
What does ‘adenomyosis belly’ refer to?
The term “adenomyosis belly” is commonly used in support groups to describe bloating or swelling in the lower abdomen caused by an enlarged uterus. This swelling often worsens around menstruation and can be both visible and uncomfortable.
How is adenomyosis diagnosed without a hysterectomy?
Today, diagnosis is usually made with imaging tests. A transvaginal ultrasound is often the first step, where a radiologist looks for changes in the uterine wall. In some cases, an MRI may be used for a clearer picture. While a hysterectomy was once the only way to confirm adenomyosis, advanced imaging has made non-surgical diagnosis possible.
Are there any natural remedies for adenomyosis?
There is no natural cure for adenomyosis, but some lifestyle changes may help ease symptoms. An anti-inflammatory diet, light exercise, stress management techniques like yoga, and heat therapy for cramps can be supportive. These should be viewed as complementary strategies, not substitutes for medical care. Be cautious of claims promising a complete cure through natural methods alone.
When should I see a doctor about possible adenomyosis?
You should seek medical advice if your periods are so heavy or painful that they interfere with your daily life, work, or relationships. Other warning signs include bleeding between periods, chronic pelvic pain, pain during sex, or persistent bloating and pressure. A consultation with a specialist can help ensure you receive the most accurate diagnosis and care.